 
It is thought to be caused by unequal inhibition of the parasympathetic pathway.Īnisocoria is an important exam finding that can be detected by an astute clinician who performs a careful and methodical pupillary exam. Over 20% of cases of anisocoria are the same in light and dark conditions and are benign, thus deemed, “physiologic anisocoria.” This condition typically presents with intermittent pupillary differences of less than 1 mm that are unchanged from light to dark and may be sporadic. 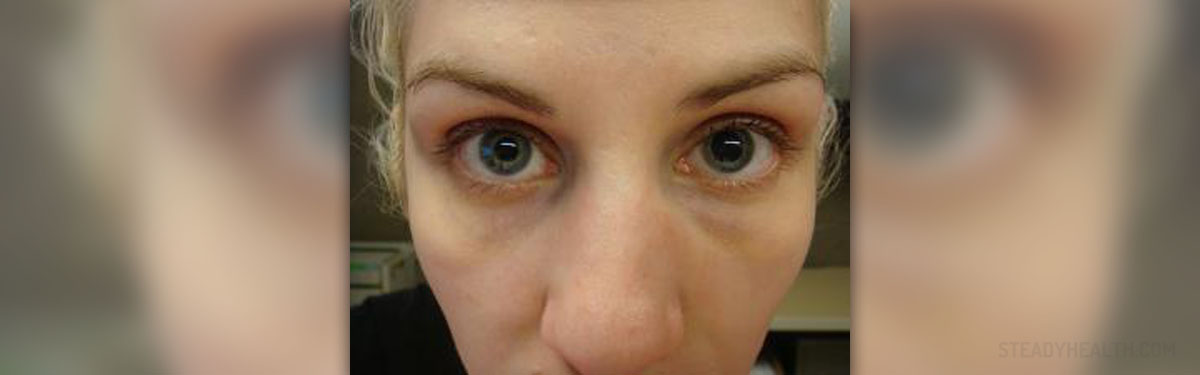
Timely identification and treatment of a carotid artery dissection-including anticoagulation-can prevent a potential embolic stroke. 
Patients with an acute-onset Horner’s Syndrome need urgent imaging of the head, neck and upper lung that would include a study capable of detecting a carotid artery dissection, such as an MRA or CTA. The most urgent and life-threatening etiology is a carotid artery dissection, but other serious causes may include a malignant lung tumor or spinal cord injury. The diagnostic challenge of a Horner’s Syndrome is that the lesion can be located anywhere along the sympathetic pathway. It is often, though not always, part of a triad of signs, the other two being an ipsilateral droopy eyelid (ptosis), and lack of sweating (anhidrosis). This presentation warrants immediately sending the patient to the emergency room for neuro-imaging and evaluation.Ī Horner’s syndrome is characterized by anisocoria greater in dark, meaning an abnormally small pupil with impaired dilation or disrupted sympathetic innervation. This could be caused by a potentially life-threatening posterior communicating artery aneurysm or impending uncal herniation. A sudden-onset dilated pupil associated with a droopy eyelid (ptosis) and abnormal eye position (strabismus – typically down and out) is highly suggestive of an acute 3 rd cranial nerve (oculomotor) palsy. The parasympathetic fibers innervating the pupil travel with the 3 rd cranial nerve, or oculomotor nerve. Checking the intraocular pressure (IOP) via a portable handheld pressure reading device, such as a Tono-pen®, would rule this in or out.Īnisocoria greater in light suggests an abnormally large pupil with impaired constriction or disrupted parasympathetic innervation. The anisocoria is greater in light suggesting impaired constriction of the right eye, or a parasympathetic defect.Ī fixed mid-dilated pupil associated with significant eye pain and redness suggests acute angle closure glaucoma. RLF = Room Light Far (focused on a distant target in light conditions). Image 1: Example of a right sided parasympathetic defect. The healthy pupil constricts to 2-4 mm in size when exposed to light and will dilate up to 4-8 mm in the dark. A halogen light is typically used to determine both direct response (the constriction of the pupil the light is being shone into) and consensual response (the constriction of the contralateral pupil when light is shone into the ipsilateral eye). The pupillary response should also be observed at near to determine if the patient has a light-near dissociation. Size of the pupil should be recorded in both light and dark conditions with the patient focusing on a target in the distance to avoid pupillary constriction associated with viewing targets at near (accommodation and the near triad). Size is most easily determined with the help of a measurement tool that includes millimeter increments, included in many near acuity cards (Figure 1). The pupils should be examined for shape, position, symmetry, reactivity, and size. Current medications: Inquire specifically about medications with autonomic effects (e.g.Medical history: Ask about strokes, sexually transmitted diseases (Syphilis), glaucoma or rheumatologic conditions.Social history: Determine if the patient has factors that would predispose them to lung pathology such as smoking.History of trauma: Inquire about trauma specifically to the eye, head or neck.Timing of Onset: Ask the patient for photos that precede the suspected date of onset as anisocoria can be noticed suddenly but may truly be longstanding or even congenital.Thus, we hope to layout a framework and approach to assist in the triage and management of these patients. Some of the associated causes of anisocoria have life-threatening implications. The difference in size between two pupils should not typically be greater than 0.4 mm, therefore most any change that the patient or clinician notices would be abnormal-whether due to a benign or malignant etiology. Home / Basic Ophthalmology Review / Pupillary ExamĪuthor: Kaitlin Smith, 4 th Year Medical Student, University of Missouri School of MedicineĪnisocoria is defined as unequal pupil sizes-occasionally first noticed by a clinician but more commonly detected by the patient and brought to the clinician’s attention. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
